Current & Recent Projects
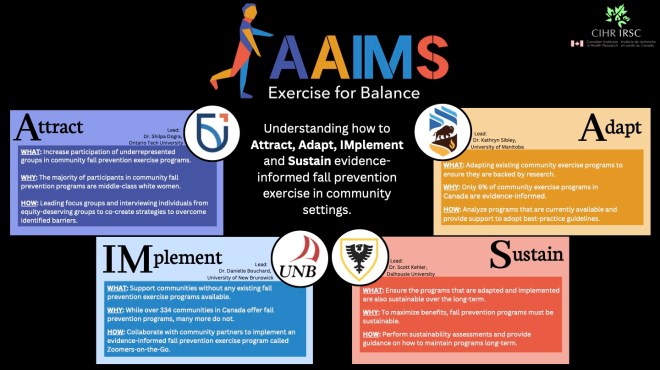
Understanding how to Attract, Adapt, IMplement and Sustain evidence-informed fall prevention exercise in community settings: The AAIMS project.
As in many high-income countries, the Canadian population lives longer than previous generations, bringing challenges at multiple levels. For instance, the prevalence and severity of falls increase with age. A robust body of evidence clearly indicates that exercises challenging balance are the most effective strategy to reduce falls, reducing the risk by as much as 51%.
Only 6% of fall prevention exercise programs in Canada are estimated to meet the recommendations: 1-providing a high challenge to balance, 2- offering at least three hours per week, and 3- offering all year long. Despite this, many community-dwellers are underserved either by not having access to, not being interested in, or by adhering to a validated program that would reduce the risk of falls.
Funded by the Healthy Cities Implementation Science Team Grant ($3.1M over 6 years), the AAIMS project purposes to advance and build capacity for the implementation science in community fall prevention exercise programming. The primary objectives are to:
1- Improve understanding of how to implement and sustain evidence-informed exercise in diverse community settings with various individuals across Canada.
2- Develop tools to support the implementation and sustainability of community exercise programs for aging adults can be used to help spread these programs.
Our main deliverable is a comprehensive planning toolkit designed to build community groups’ capacity to attract equity-deserving groups, adapt a program to make it evidence-informed, implement an evidence-informed program or sustain existing or newly implemented programs.
Our approach to the AAIMS project is grounded in integrated knowledge translation– a collaborative research approach that involves the “end users” of research in the governance and conduct of research with the aim of producing relevant and usable findings. Informed by our partners within diverse settings, structures, and contextual needs, we have created four related research streams that draw on a multiple case study design.
Advancing the Science of Integrated Knowledge Translation with Health Researchers and Knowledge Users: Understanding Current and Developing Recommendations for Integrated KT Practice
Partnerships between researchers and knowledge users is key to producing evidence that is more relevant to its users. In health research, integrated Knowledge Translation (iKT) is a collaborative research approach in which research users (also called knowledge users), such as people with lived experiences of a health condition, families, health professionals and decision-makers, are involved throughout the research process. It makes knowledge translation more meaningful and effective by producing research that is more relevant and likely to be used.
Using mixed methods approach, the overall goal of this CIHR-funded project is to examine how health research partnerships have been conducted and evaluated in Canada. There are two key objectives of this project: 1) to develop a comprehensive understanding of current iKT practice; and 2) to make recommendations for conducting and evaluating iKT.
The research team includes both researchers and knowledge users –– including decision-makers, clinicians, and patient partners –– from across Canada who bring varied expertise to the project. The long term goal of this project is to improve the health of people across Canada by ensuring the latest research is quickly incorporated into everyday health care practice and policies.